No advantages having a CS once eligible for vaginal birth
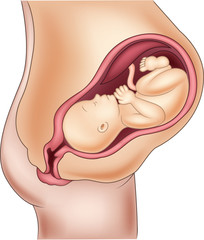
Cesarean sections (CS) are generally considered safe and in some situations life-saving. However, they carry additional risks such as severe bleeding, scarring, infections and more longer-lasting pain, compared with a vaginal birth. The bowel or bladder can also be injured during a CS operation and blood clot (thrombosis) risk is higher. Women should be as informed as possible about their childbirth options, so they can have an informed decision in the process. During vaginal delivery, muscles squeeze out fluid from newborn’s lungs reducing the risk of breathing problems. The embryo receives an early dose of good bacteria in the birth canal that accelerate their immune systems and protect their intestinal tracts. Women who had CS are less likely to begin early breastfeeding than women who had a vaginal birth. The recovery period after delivering is also longer because a woman may have more pain and discomfort in her abdomen as the skin and nerves surrounding her surgical scar need time to heal. Once a woman undergoes a CS, she is more likely to have a CS in her future deliveries. She may also be at greater risk of future pregnancy complications, such as uterine rupture, which is when the CS scar in her uterus ruptures, and placenta abnormalities. The risk for placenta problems continues to increase with every CS a woman has.
Studies find that a vaginal delivery covers a baby with beneficial bacteria. Babies born vaginally have a decreased risk of certain immune system disorders, including asthma and allergies, compared with those born by CS. Vaginal delivery exposes babies to several beneficial bacteria, including Lactobacillus, found mainly in the vagina and colonizes the newborn’s intestine, helping in the digestion of milk. The vast majority of microbes are helpful and even necessary for body functions. The microbes in the gut determine how efficiently a person processes nutrients, and help to regulate our metabolism. During pregnancy, the composition of bacteria in a woman’s vagina changes so there is a higher concentration of Lactobacillus. A baby born by CS will miss out on immediately acquiring these beneficial bacteria. The mode of delivery has been associated with differences in intestinal microbes even 7 years after delivery.
Gut colonization by microbes is delayed in CS delivered babies, which may explain in part why these infants face difficulties fighting off infections. Immediately after birth, the establishment of gut bacteria can affect the development of the immune system. A baby’s gut microbiota can also affect its disposition in the first weeks and months of life. Infants with colic pains have more bacteria that are known to produce gas, whereas anti-inflammatory bacteria that live in the vaginal canal are more common in colic-free infants. More and more scientific evidence demonstrate the connections between the gut bacteria in infants and an increasing number of health problems that are more common in children born by CS, such as obesity, asthma, allergies, type 1 diabetes, food allergies, eczema, and celiac disease.
Trials to transfer the vaginal flora microbiota to the newborn mouth by vaginal swabs immediately after CS in order to imitate the vaginal delivery fail to prove equal benefits. Microbiological investigations of infant faeces born by CS demonstrated poor microbiota infestation and lower immunity indices once compared to newborns delivered vaginally.
The health benefits gained by mothers and babies after trial of vaginal delivery are enormous. Even in cases that trial of vaginal delivery will end by CS due to labour difficulties the transmission of microbiota and infant gut colonization by microbes is evident.

